NRH Acquired Brain Injury Programme
The National Rehabilitation Hospital (NRH) provides comprehensive inpatient and outpatient services to patients who, as a result of an accident, illness or injury, have acquired a physical or cognitive disability and who require specialist medical rehabilitation.
The Consultant led Brain Injury Programme Programme at the NRH is backed by experience, clinical expertise and a solid reputation for excellence.
The Interdisciplinary Team within the Brain Injury Programme provides specialised rehabilitation treatment and care, designed to assist people with a diagnosis of Acquired Brain Injury (ABI):
- Adjust to their injury
- Achieve the safest possible level of physical independence
- Participate socially and in the community
The NRH has developed a full continuum of care for people with Acquired Brain Injury
Read more
This continuum of care includes:
- Brain Injury Comprehensive Integrated Inpatient Rehabilitation Programme
- Brain Injury Outpatient Rehabilitation Programme
- Brain Injury Home and Community Based Rehabilitation Programme
- Brain Injury Vocational Services (the Rehabilitative Training Unit)
This continuum of care ensures that all individuals can receive the most appropriate programme of care based on their injury and their individual rehabilitation needs.
With primary inpatient and outpatient Brain Injury rehabilitation services provided at the NRH, the comprehensive Brain Injury Programme includes a consulting service to:
- Beaumont Hospital
- The Mater Hospital
- St. Vincent’s University Hospital
- Tallaght University Hospital
Additional sessions for continuing rehabilitation for those whose brain injury results in a ‘slow to recover’ process are delivered at:
- Royal Hospital Donnybrook
- Peamount Hospital
The programme aims to discharge all patients after they have achieved their desired rehabilitation goals and have received maximum benefit from the programme.
Show less
Rehabilitation Team in the Brain Injury Programme
Read more
Patient care and treatment for the Brain Injury Programmes is delivered by interdisciplinary teams (Medical, Nursing, Health and Social Care Professionals), with clinical responsibility led by Dr Sabrina McAlister, Medical Director for the BI Programme.
In addition, Consultants in Rehabilitation Medicine who provide a service to these Programmes include:
- Prof. Jacinta Morgan
- Dr. Raymond Carson
- Dr. Paul Carroll
Kate Curtin is the Programme Manager for the Brain Injury Programme
At the NRH, the Brain Injury and Stroke Specialty services access the full complement of support from:
- Medical
- Nursing and clinical support
- Therapy services
- Patient Services (administration)
Input is also required from Neuropsychiatry, Gastroenterology, Endocrinology, Ophthalmology, and ENT.
Show less
Brain Injury Programme Scope of Service
Link to BI Programme Scope of Service.
Referrals to the Programme
Link to referral criteria and medical Referral Form.
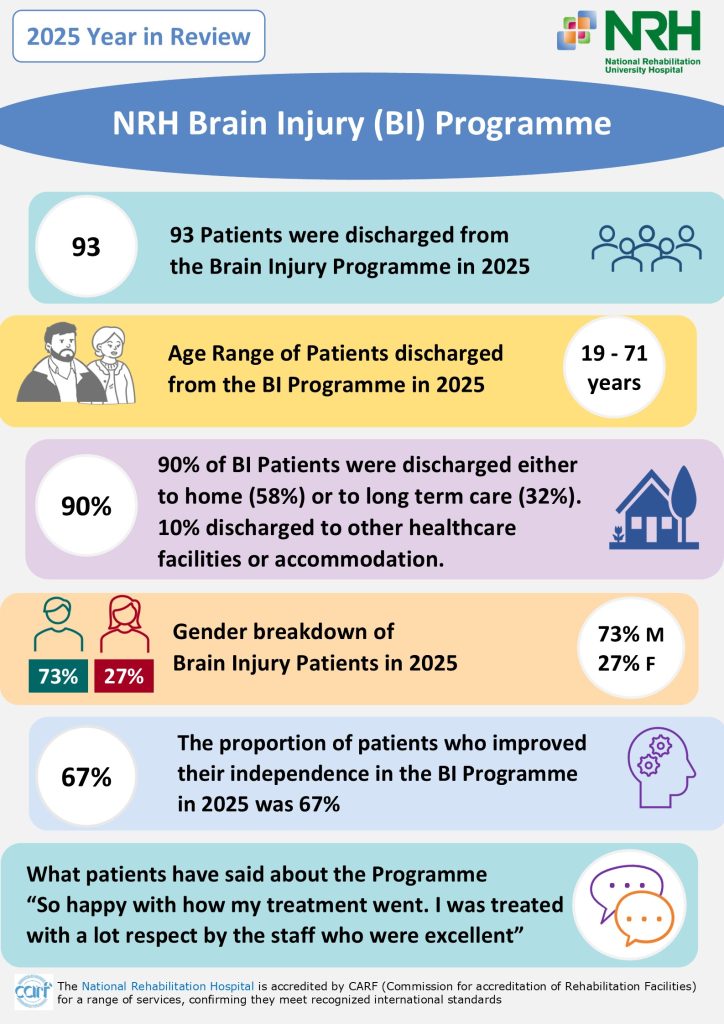
Demographics, Activity and Outcomes for Inpatient Services